female investigation
female investigation
Everything about the procedure of female investigation
during your fertility consultation
Saline infusion sonography (SIS) or sonohysterography entails saline injection into the uterine cavity under ultrasound guidance. The sensitivity of sonohysterography is significantly better than that of a transvaginal ultrasound on all kinds of intrauterine pathology, such as polyps and fibroids. It also acts as a mock embryo transfer, giving us valuable information in your fertility consultation regarding the ease of accessing the uterine cavity.
A saline infusion sonography (or aquascan) is done at our clinic, usually during your first fertility consultation with us. You can have an aquascan after your period has finished but before ovulation. Depending on the findings, you may be referred to have a hysteroscopy or laparoscopy.
The role of the immune system in terms of implantation failure and recurrent miscarriages has received much attention by the scientific community in recent years. The immune system plays a key role in reproductive medicine. It helps our body to distinguish self from non-self and protects us against infections and abnormal or malignant cells. Complex interactions between the developing trophoblast of the future embryo and the endometrium occur, which finally lead to a state of maternal-foetal tolerance. Derangements of the immune system can prevent implantation or cause a miscarriage.
A comprehensive panel of tests is currently available that examines different components of the immune system. At Serum, we provide immune testing to patients when this is indicated by their medical and fertility history mostly during your fertility consultation in Greece or after failed IVF treatments.
HLA-DQ Alpha Testing:
This test determines if partners share tissue proteins that are too similar (tissue-type compatibility). If compatibility is high, the female will not produce antibodies that protect the foetus from an immune attack and therefore, the foetus is prone to rejection.
Leukocyte Antibody Detection (LAD)
This test measures the level of blocking antibodies in a woman’s blood. If the level of such antibodies is low, there is a high possibility that the foetus will be rejected.
Natural Killer Cell Assay
NK cells are lymphocytes which mediate cell destruction (cytolysis), produce cytokines and mediate natural resistance against tumour cells. With the NK cell assay we separate the NK cells from the woman’s blood and mix them with target cells to investigate their critical role in the preparation of the endometrium for the embryo.
Blood Clotting Disorders
These are conditions which lead to a hypercoagulable state and are associated with blood clots in the very small arteries and blood vessels. The specific tests are:
Antiphospholipid antibodies (Lupus anticoagulant, antibodies against cardiolipin, etc.)
Inherited Thrombophilias (Factor V Leiden gene mutation, protein C & S deficiency, MTHFR 677 T mutation, etc.)
Spontaneous abortion or miscarriage is clinically recognised as the non-induced loss of a pregnancy before 20 weeks of gestation. Recurrent miscarriage is defined as loss of two or more consecutive pregnancies. Overall, 50-75% of miscarriages are due to sporadic chromosomal abnormalities and hence occur by chance. The most common ones are trisomies, such as Down’s syndrome (Trisomy 21). Maternal ageing is associated with an increased risk of miscarriage, which reflects a rising prevalence of oocyte aneuploidy. Karyotype of both partners or the abortus can provide evidence towards the type of anomaly or may suggest a non-genetic cause when normal. IVF with pre-implantation genetic diagnosis (PGD) and selected transfer of euploid embryos is an established treatment for couples when one partner is a carrier of chromosomal anomaly.
Anatomic anomalies of the uterus predispose an increased risk of pregnancy loss and can be identified by sonohysterography or the traditional hysterosalpingogram (HSG) or hysteroscopy. Septate uterus is the most common anomaly and the one most closely associated with recurrent pregnancy loss. This malformation can be corrected via hysteroscopy. Uterine leiomyomas/fibroids, especially those that protrude or displace the uterine cavity, can be associated with pregnancy loss.
Pregnancy outcomes are much improved after hysteroscopic removal of intrauterine adhesions. At Serum, we have pioneered the performance of “implantation cuts” at the fundus of the uterus which has resulted in a significant increase in implantation rates, and it can be easily performed during your fertility consultation in Greece.
Maternal immune recognition and response play an important role in normal pregnancy and may be a cause of an otherwise unexplained recurrent pregnancy loss. There is a lot of ongoing research into this area in recent years and Serum offers to its patients an extensive testing and treatment for immune issues evaluated during the fertility consultation.
Inherited and acquired thrombophilias resulting from mutations in clotting factors have emerged as a potentially important cause of recurrent pregnancy loss. Pathologic thrombosis results from an imbalance between coagulation and fibrinolysis. At Serum, we screen for inherited thromobophilias women who have an otherwise unexplained recurrent pregnancy loss or have previous history of pregnancy complications that have resulted from thrombosis or failure of the placenta (such as preeclampsia and intrauterine growth restriction).
Endocrine factors are another cause of recurrent pregnancy loss. Thyroid disorders are easy to identify and treat and can be diagnosed by TSH measurement. Evaluation of blood glucose and insulin tolerance test are indicated for women with known or suspected diabetes. The risk of miscarriage is increased among women with polycystic ovary syndrome and insulin resistance and may be significantly reduced by treatment with metformin.
Chronic infections of the reproductive tract are an important factor for infertility and pregnancy loss. At Serum, we perform Microbiome Molecular Analysis (MbMA) of period blood tissue that can be easily collect a biopsy once you visit us. The test is carried out in collaboration with a specialised laboratory in Athens. This test has very high sensitivity for diagnosing chronic infections such as Chlamydia, Ureaplasma or Mycoplasma and various significant bacteria such as Streptococcaceae, Staphylococcaceae, and Enterobacteriaceae species, while more importantly evaluates the levels of Lactobacillaceae species. If an abnormality is identified, we provide our patients with antibiotic and probiotic treatment before an intended IVF treatment cycle or even prior to a natural conception attempt.
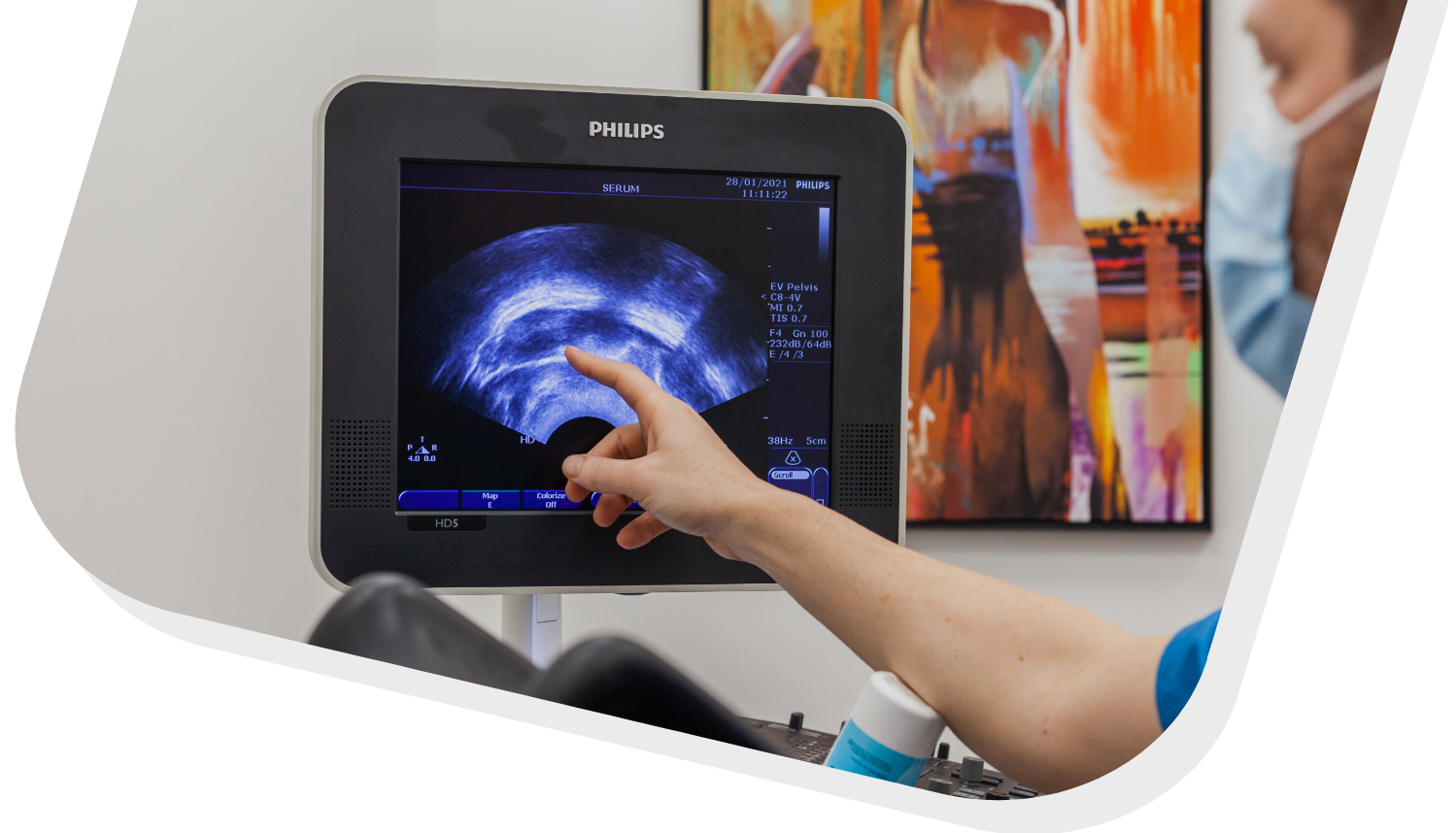
Gynaecological ultrasonography, the first step of your fertility consultation, refers to the application of medical ultrasonography to the female pelvis (with focus to the uterus, ovaries, adnexa, bladder, and the Pouch of Douglas). The examination can be performed transabdominally (with a full bladder which acts as an acoustic window to achieve better visualization) or transvaginally. Transvaginal imaging provides better resolution of the pelvic organs, whereas larger lesions reaching into the abdomen are better seen transabdominally. Ultrasound is an invaluable tool in everyday practice as it is used to diagnose gynaecologic problems such as uterine polyps, fibroids, adenomyosis, ovarian cysts and adnexal masses, including ectopic pregnancies. It is routinely used to follow up a natural menstrual cycle and can provide evidence for ovulation.
Specifically in IVF treatment protocols, the ultrasound scan provides valuable information such as the antral follicle count (AFC), while allows monitoring the response of the ovaries to controlled ovarian stimulation in women that undergo IVF (own egg programmes). In your first fertility consultation in Athens, you will have this scan in order to form your stimulation protocol. In donor egg cycles, the ultrasound is used to evaluate the response of the endometrium (internal lining of the uterus) to exogenous oestrogens.
A basic laboratory workup is an essential initial part in the evaluation of infertility and offers valuable information. The results of these tests provide clues on the aetiology of the infertility problem and function as a guide to the next steps in management. You can easily have this examination during or prior to your fertility consultation.
FSH
FSH along with LH (the so-called gonadotropins) are hormones produced by the pituitary gland. They regulate the secretion of the ovarian hormones such as oestradiol. FSH measured on menstrual cycle (day 3) is most commonly used to evaluate the ovarian reserve.
Oestrogens
They are important hormones of the female reproductive system with a wide range of effects on many organs in the body. Oestrogens facilitate the growth of ovarian follicles, and they have an important role in the cyclic changes of the endometrium, cervix, and vagina. 98% of the body’s oestrogens are derived from the ovary. Oestradiol level is commonly checked on day 3 of menstrual cycle (along with FSH) to evaluate ovarian function.
Anti-Mullerian hormone (AMH)
AMH is produced by the very small (non-selected) follicles of the ovaries. A serum AMH assay can be used to identify patients with low ovarian reserve and polycystic ovarian syndrome.
TSH & Prolactin
TSH is an important indicator of thyroid function, while prolactin is a protein secreted by the pituitary gland and its main role is milk production. Since thyroid dysfunction and hyperprolactinemia are associated with menstrual irregularities and infertility, a serum TSH and prolactin level should always be checked and corrected prior to initiating therapy.
Pre-screening for Infections
According to the Greek Law, we have to obtain a panel of blood tests for infectious diseases before any IVF treatment. These include test results for hepatitis B, hepatitis C, HIV type I-II and syphilis.
Immunology tests
A variety of blood tests for immune issues are available. For more information, CLICK HERE
Hysteroscopy is the gold standard for diagnosing and treating intrauterine pathology which may adversely affect fertility. Apart from the ovarian activity and the sperm quality, the third parameter we focus on in your fertility consultation at Serum is the uterine cavity.
Examples include:
Developmental anomalies of the uterus, such as a uterine septum.
Hysteroscopic septum resection can usually be performed as a relatively straightforward and quick procedure.
Hysteroscopy is the method of choice for treatment of intrauterine adhesions and is both safe and effective when performed by expert gynaecological surgeons.
Endometrial polyps are almost always benign endometrial growths that protrude into the uterine cavity. Polyps may interfere with implantation, cause local inflammation or distortion of the uterine cavity. They can be easily removed via hysteroscopy (hysteroscopic polypectomy).
At Serum, we have pioneered a procedure called hysteroscopy with implantation cuts, a procedure that can be easily arranged in your fertility consultation. During a routine hysteroscopy, the doctor uses the operative scissors to perform small cuts at the bottom of the uterus (fundus) along a line which extends between the entrances of the tubes on each side. The depth of the cuts extends down to the healthy tissue. The fundus of the uterus is the implantation site of the embryo and by doing this technique we increase the probability for the embryo to implant.
Laparoscopy
Laparoscopy and dye test is the gold standard for the evaluation of tubal factor infertility. Injection of a dilute dye through a cannula attached to the cervix during laparoscopy permits evaluation of the tubal patency.
On top of that, Laparoscopy provides a panoramic view of the pelvis and hence can identify pathologies such as adhesions or endometriosis that can adversely affect fertility. Most importantly, laparoscopy offers the opportunity to “see and treat” a wide range of pathologies, such as adhesions, ovarian cysts, hydrosalpinges, endometriotic lesions and fibroids. At Serum, we do laparoscopy along with hysteroscopy at the same time. You can arrange this in advance of your fertility consultation or decide it after meeting our specialists.





